Freezing Hunger Signals Offers Promising New Treatment for Weight Loss
April 17, 2018

 Play
Play

Emory interventional radiologist J. David Prologo, MD, FSIR, ABOM-D is making headlines as lead author of a preliminary study testing image-guided treatment for weight loss.
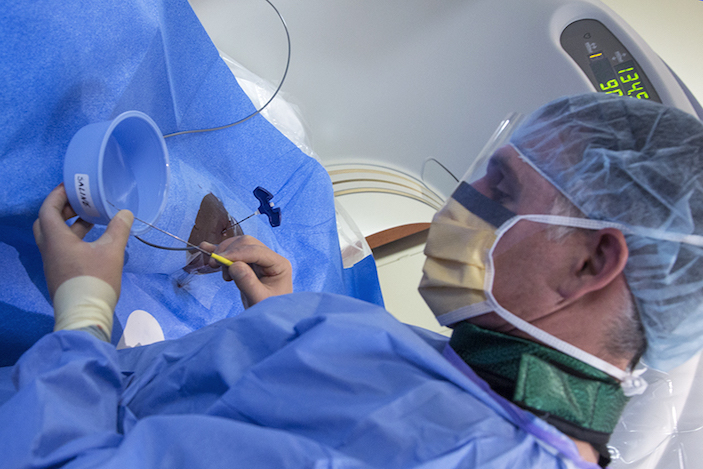
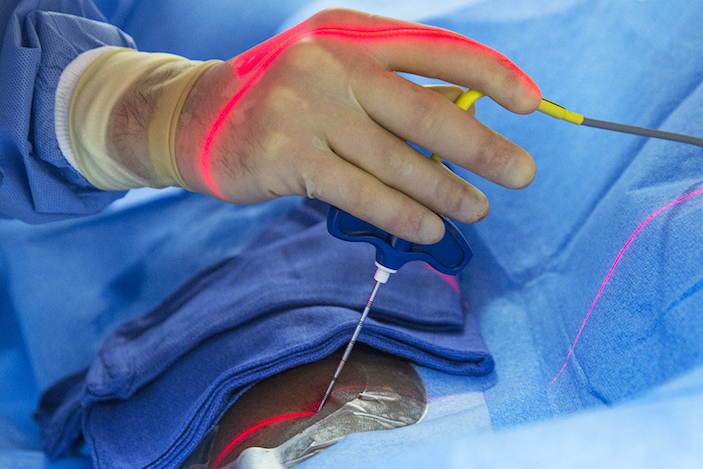
As part of a feasibility study, ten men and women categorized as obese were sedated and then, using CT guidance, radiologists inserted a needle filled with a freezing gas into a nerve called the vagus nerve. Freezing the nerve prevented it from sending hunger signals to the brain.
Ninety days after the 30-minute process, 53% of the treated patients reported “very much less appetite,” 30% reported “much less appetite” and 17% reported “somewhat less appetite.” The patients lost an average of 3.6% of their initial total body weight corresponding to about a 14% reduction in excess body mass index (BMI). No adverse events occurred during the 90-day period and no procedure-related complications were noted.
Not only did the results of the study generate buzz when presented at the Society of Interventional Radiology’s 2018 Annual Scientific Meeting in March, the findings resulted in a deluge of patient queries after being featured nationally by TIME, The Chicago Tribune, U.S. News and World Report, MedPage Today, WABC-TV, Science Daily, Today, and locally by the Atlanta Journal-Constitution.
Dr. Prologo discusses the procedure as well as the research study in a new video produced by Emory Radiology’s Communications and Creative Services team and available here on YouTube. The video also features the first patient enrolled in the study discussing her relationship with food and the power and promise of participating in the study.
Dr. Prologo is excited about the next phase of research and even more passionate about what a game-changer this procedure could be for patients. “The primary take-home point here is people should not be shamed for their inability to lose weight,” he says. “We as physicians in the scientific community realize there’s a real biological backlash that happens when people embark on mainstream diets, embark on calorie restriction. We know something real is happening in your body and we want to put an end to fat shaming altogether.”
For more information regarding this study, please click here.